What is ADHD?
|
Attention-deficit/hyperactivity disorder (ADHD) is neurological disorder that is broadly characterized by individuals who display excessive motor activity, inattention, and impulsivity. Someone with ADHD will have a harder time staying on task and staying focused on a goal, and this is not due to a lack of knowledge or comprehension. They also can be hyperactive and constantly be fidgeting, tapping, or talking at inappropriate times. They can also be excessively impulsive and make rash decisions in order to obtain an immediate reward without thinking of the long term consequences. In the United States, about 11% of children aged 4-17 years old have been diagnosed with ADHD since 2011. Boys aged 4-17 are more likely to have ADHD at 13.2%, and girls with 5.6%. (1). In 1902, a British pediatrician, Sir George Frederic Still, gave the first medical diagnosis of ADHD. He first described the children is having a “defect of moral control as a morbid manifestation, without general impairment of intellect and without physical disease” (2).
|
What causes ADHD?
There is not one universal root cause to ADHD. People with ADHD can fall on a spectrum of symptoms, and commonly associated with other psychiatric disorders. Imaging of children's brains with ADHD have been shown to be significantly smaller than that of unaffected controls. The prefrontal cortex, cerebellum, and basal ganglia are specific areas that show a reduction in white matter (3). The prefrontal cortex plays an important role in ADHD as it is involved with decision making, personality development, impulsivity, and planning. Individuals with ADHD have difficulty moderating these behaviors. ADHD has been reported to have a heritability of up to 0.8, showing that genetic factors in ADHD are very deterministic to the disease (4). There are many possible genetic markers that have shown to be significantly related to ADHD and cross talk between these genes is complex. Genes important in cell signaling and synaptic activity are especially of interest in ADHD. LPHN3 is a new gene of interest that has been linked with ADHD and substance abuse.
How is LPHN3 associated with ADHD?
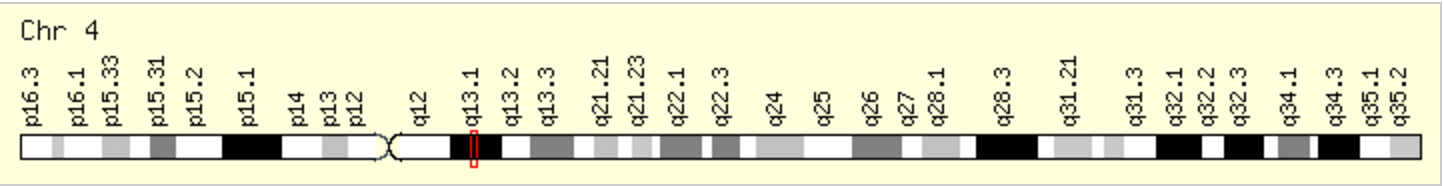
Latrophilins (LPHNs) are adhesion G protein-coupled receptors. They are located in the transmembrane and are involved in cell signaling; and sense extracellular signals such as neurotransmitters. There are three latrophilin genes LPHN-1, LPHN-2, and LPHN-3. LPHN-1 and LPHN-3 are expressed in the brain, while LPHN-2 is expressed in non-neural tissues. LPHN-3 has been specifically linked with ADHD and loss of LPHN3 gene function has been identified to impair the development of dopamine-mediated mechanisms (4). Several single-nucleotide polymorphisms (SNPs) in LPHN-3 have been associated with ADHD. that affect splicing of LPHN-3. One SNP, rs1397548, ends up in the deletion of exon 15. This deletion results in a shortened protein with altered functions that has been associated with ADHD (2). SNPs at LPHN-3 has been shown to impair the binding of teneurin-1. Teneurin-1 is crucial in the development of neonural pathways, which LPHN-3 was found to regulate influence the development and number of neural synapses. Variants in LPHN-3 show decreased amounts of brain synapses, which is a phenotype of ADHD (5).
How is ADHD treated?
|
It is recommended that behavior therapy is tried first before any medication is used. Since ADHD can be very complex and individual symptoms can vary it is best to try to understand the individual before prescribing medications. Behavior therapy can come from a combination of a therapist and a parent. It is aimed at helping a child with managing their behaviors, such as: learning ways to control their behaviors, improve self control and self esteem. Behavior therapy should always be the first line of defense.
Medications are another effective and common way to treat ADHD. Stimulants are the most common form of treatment for someone with ADHD. Many of these stimulants, such as the common methylphenidate (MPH), target the dopaminergic systems to help manage emotion dysregulation in ADHD. |
|
Text References:
(1) Holland, K., & Riley, E. (n.d.). ADHD by the Numbers: Facts, Statistics, and You. In ADHD (Attention Deficit Hyperactivity Disorder). Retrieved September 4, 2014, from http://www.healthline.com/health/adhd/facts-statistics-infographic (2) Molecular Psychiatry (2010) 15, 1053–1066; doi:10.1038/mp.2010.6; published online 16 February 2010 (3) Facts About ADHD (2016, November 16). In Attention-Deficit / Hyperactivity Disorder (ADHD). Retrieved from https://www.cdc.gov/ncbddd/adhd/facts.html (4) Woelfle, R., D’Aquila, A. L., Pavlović, T., Husić, M., & Lovejoy, D. A. (2015). Ancient interaction between the teneurin C-terminal associated peptides (TCAP) and latrophilin ligand-receptor coupling: a role in behavior. Frontiers in Neuroscience, 9, 146. http://doi.org/10.3389/fnins.2015.00146 (5) O’Sullivan, M. L., Martini, F., von Daake, S., Comoletti, D., & Ghosh, A. (2014). LPHN3, a presynaptic adhesion-GPCR implicated in ADHD, regulates the strength of neocortical layer 2/3 synaptic input to layer 5. Neural Development, 9, 7. http://doi.org/10.1186/1749-8104-9-7 (6) K. Drabikowski, A. Trzebiatowska, R. Chiquet-Ehrismann. (2005). Ten-1, an essential gene for germ cell development, epidermal morphogenesis, gonad migration, and neuronal pathfinding in Caenorhabditis elegans. Developmental Biology, 282, pp. 27–38 Figure 1: https://assets.rebelcircus.com/blog/wp-content/uploads/2016/02/32413.jpg Figure 2: https://www.degruyter.com/view/j/tnsci.2016.7.issue-1/tnsci-2016-0004/graphic/j_tnsci-2016-0004_fig_002.jpg |
Image References:
Cover image: https://i.ytimg.com/vi/VIcGRffuMLg/maxresdefault.jpg Image 1. http://study.com/cimages/multimages/16/hiperactividad_large.jpg Image 2. http://southcountychildandfamily.com/wp-content/uploads/2013/11/chatchat-1.jpg Image 3. http://addadhdblog.com/wp-content/uploads/methylphenidate.jpg Image 4. http://cognitivetherapysf.com/wp-content/uploads/2014/04/CBT-photo.jpg Figure 1. http://www.genecards.org/cgi-bin/carddisp.pl?gene=ADGRL3 |
|
Author: Sean Brennan Email: [email protected] Institution: University of Wisconsin - Madison Course Website: www.genetics564.weebly.com Last Updated: May 13, 2017 *site is under construction* |
|